7 lessons about coronavirus that CU Boulder scientists helped discover
From the moment CU Boulder pivoted to remote learning in March 2020, researchers across campus began deploying their scientific expertise to not only prepare campus for reopening, but to also understand all that they could about the virus.
As of March 1, 2021, campus scientists had launched 34 COVID-19-related research projects and had nearly 100 more in the works. Topics ranged from: how the virus spreads in orchestras to how it influences mental health and how best to distribute vaccines. Findings from this research have already shaped public policy around the globe.
There’s still a lot to learn, but here’s a glimpse at what we found out so far.
It was here before we knew it
Colorado officially chalked its first positive case of COVID-19 on March 5, 2020. But the coronavirus was likely hiding out in the Rocky Mountains long before that.
That’s the conclusion of research led by the state’s COVID-19 Modeling Team, of which David Bortz, an associate professor in the Department of Applied Mathematics at CU Boulder, is a member. For nearly a year, Bortz and his colleagues on this epidemiological dream team have employed their mathematical skills to provide state officials with timely public health guidance around the pandemic, briefing Gov. Jared Polis weekly.
In their latest work, they drew on data from the early spread of COVID-19 to back-date the virus’ arrival close to home. The coronavirus, they estimated, may have been in the state since January—weeks before an out-of-state skier tested positive in Summit County.
Read more: Mathematician on the front lines of Colorado’s coronavirus response
It spreads best through the air
[video:https://www.youtube.com/watch?v=AGQYlrXzVJQ]
SARS-CoV-2, the virus that causes COVID-19, spreads between people in three ways: through aerosols, respiratory droplets and by touching contaminated surfaces and then touching one’s face.
But no, we don’t need to wipe down our groceries. Contrary to initial warnings, there is no documented evidence of transmission by contaminated surfaces (known as fomites) according to Jose-Luis Jimenez, professor in the Department of Chemistry and a fellow in the Cooperative Institute for Research in Environmental Sciences (CIRES).
There is, however, an abundance of evidence that SARS-CoV-2 is transmitted most often through aerosols—especially in crowded, indoor spaces with poor ventilation like restaurants, bars and gyms.
These microscopic droplets of liquid are produced when we breathe, talk, cough and sing—and an even smaller COVID-19 viral particle can hitch a ride on them. Unlike larger droplets produced when we cough or sneeze (which drop to the ground quickly), aerosols float like smoke and can travel more than 6 feet.
While the Centers for Disease Control and Prevention (CDC) did not openly acknowledge the role of aerosols in COVID-19’s spread until October, the World Health Organization (WHO) updated its guidance in July in response to a letter signed by hundreds of scientists across the world, including Jimenez and Shelly Miller, professor in the Paul M. Rady Department of Mechanical Engineering.
Research published by Miller and Jimenez in September further confirmed this theory, concluding that singing indoors and unmasked can swiftly spread SARS-CoV-2 virus through airborne particles. “Aerosol transmission is playing a major role in driving this pandemic and especially to superspreading events,” concluded Jimenez.
Read more: Experts weigh in on airborne transmission of COVID-19, Singing unmasked, indoors spreads COVID-19 through aerosols
Masks, on faces and instruments, keep people safe
[video:https://www.youtube.com/watch?v=p3l9_-mL4Fo]
In addition to social distancing and washing one’s hands, we now know that wearing a mask is one of the most important things a person can do to prevent the spread of COVID-19. Masks trap viral particles attached to aerosols and larger droplets as they leave your mouth or as you encounter those produced by other people.
But here’s a question: if people talking and singing emit aerosols, can their musical instruments? The answer is "yes," according to CU Boulder research. This fall, Miller led a team of researchers from across the university to find out how musical ensembles around the world can continue to safely perform music together during the pandemic.
“We're finding that masking an instrument could be just as important as masking a human,” said Jean Hertzberg, associate professor of mechanical engineering and one of the researchers involved with the study.
Read more: Aerosol research instrumental in getting musicians back to playing safely
Ventilation is key
Miller also knew right away that improving ventilation in indoor spaces would be key to reducing the spread of COVID-19. This can be done by bringing in fresh air from outside or removing the virus from the air inside the building. We learned how important it is to open our windows, install air filters, turn on exhaust fans and limit our time inside with others.
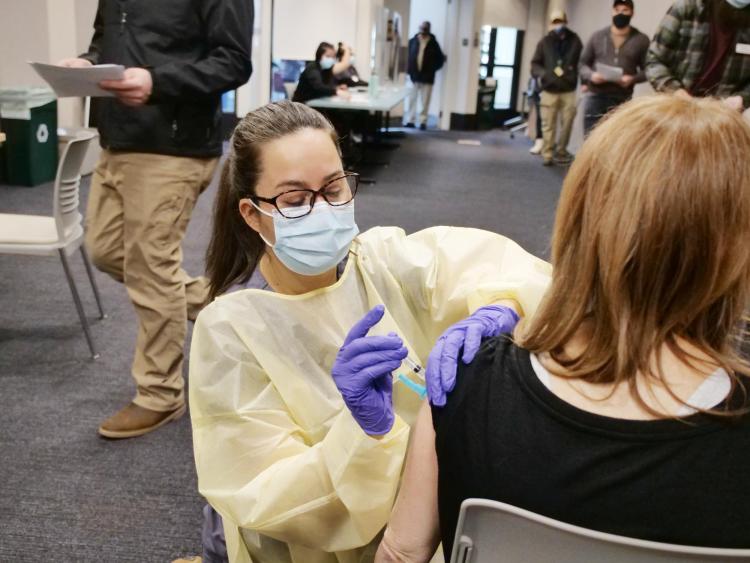
From top to bottom: Shelly Miller (left) and graduate student Teyha Stockman (right) fit a bell cover over a clarinet; Benton Hart, preventative maintenance tech, replaces old air filters in the Indoor Practice Facility; COVID-19 Johnson and Johnson vaccination clinic at CU Boulder; Students participate in a Greek mask review in Tamara L. Meneghini-Stalker’s Studio 4 class. (Credits: Glenn Asakawa, Casey A. Cass, Patrick Campbell/CU Boulder)
To improve ventilation on campus, Miller and many staff members worked around the clock as part of a new Facilities Task Force to ensure that students, faculty and staff would breathe the safest possible air indoors on campus. To date, there have been no documented cases of COVID-19 from classroom instruction on campus. Prioritizing ventilation is also key to keeping K-12 schools safe as they plan for reopening in 2021. (Learn more about recent work by CU Boulder researchers in environmental engineering in Denver Public Schools).
How do you know if a space is well-ventilated? Researchers have an answer for that, too: One simple trick is to measure the concentration of carbon dioxide because we exhale this gas when we breathe.
“Carbon dioxide accumulation in a space is a sign of poor ventilation, and most of the COVID-19 transmission is happening in crowded, poorly ventilated environments,” said Miller.
Read more: Why better ventilation is key to limiting COVID-19 spread on campus
Vaccinating older people first saves lives
This month, the lines to get a COVID-19 vaccine in Colorado have been long—and many of the people waiting have been elderly, more vulnerable state residents.
When it comes to maximizing public health, vaccinating those older people first may be the best policy, said Daniel Larremore, a computational biologist in the BioFrontiers Institute at CU Boulder.
In January, he and graduate student Kate Bubar published a study in the journal Science that used mathematical models to test out possible strategies for vaccinating people around the world. The team created scenarios, for example, in which health officials gave the first vaccines to adults age 20 to 49—or even adopted a first-come, first-served policy.
Vaccinating adults 60 or above first seemed to be the most effective approach for lowering mortality rates. When it comes to COVID-19, “age is the strongest predictor of vulnerability,” Larremore said.
Read more: Who should get the first COVID-19 vaccines? Global study provides insights
Dorms and classrooms are safer than we thought
To date, not a single case of COVID-19 has been confirmed to have spread in a classroom on the CU Boulder campus.
And, according to a new, yet-to-be published study led by COVID Scientific Director Kristen Bjorkman, only about 20% of students who tested positive for the virus while living in residence halls in the fall transmitted it to their roommate.
“This is important for us and other universities to know because it tells us we can continue to offer on-campus housing and roommate pairing,” she said.
The study also found that those who did transmit it to their roommate had viral loads—the amount of virus particles in their saliva sample—seven times greater than those who didn’t.
The takeaway: Viral load may matter more than we realized when it comes to how contagious someone is.
Read more: 2% of people carry 90% of COVID-19 virus, and roommates are safer than you think
We need to flatten the mental health curve, too
We haven’t just learned about viruses this past year—we know that fear, misunderstanding and loneliness can also be dangerous to our health.
From the beginning of 2020, fear played a role in not only how we protected ourselves from the virus, but how we treated each other. For Jennifer Ho, professor of ethnic studies and director of the Center for Humanities and the Arts, the racism directed towards Asian Americans in the U.S. as a result of COVID-19 originating in China was not only concerning, it was personal.
Due to a sudden surge of violent attacks on Asian Americans in the spring of 2020, as well as the death of George Floyd in Minneapolis that May, Ho partnered with PhD candidate Shawn O’Neal to create a free online course all about anti-racism on CU Boulder’s Coursera platform.
June Gruber, associate professor of psychology and neuroscience and director of the Positive Emotion and Psychopathology Laboratory, taught us that it’s OK to not feel OK all the time.
"Emotional diversity is a really natural and important part of being human," said Gruber, who recentl launched a new, free online course #talkmentalillness to raise awareness . "It is not only acceptable to feel sad and frustrated and exhausted right now, it is perfectly appropriate. These emotions serve a purpose of keeping you in touch with the unusual world we are living in."
She also reminded us of the importance of being in this together, even though we often need to stay physically apart.
Going forward, with the curve flattening in terms of hospitalizations, Gruber said we should keep another curve in mind:
"We must pay attention to the ongoing and future mental health curve and repurcussions impacting everyone who has endured these stressful times."
Read more: Anti-Asian discrimination amid pandemic spurs Jennifer Ho to action, Free anti-racism course opens door to 'some very difficult questions', Flattening the mental health curve is the next big coronavirus challenge
Daniel Strain and Lisa Marshall contributed to this story.