If I get the shot, can I still get COVID-19? Answers to common vaccine questions

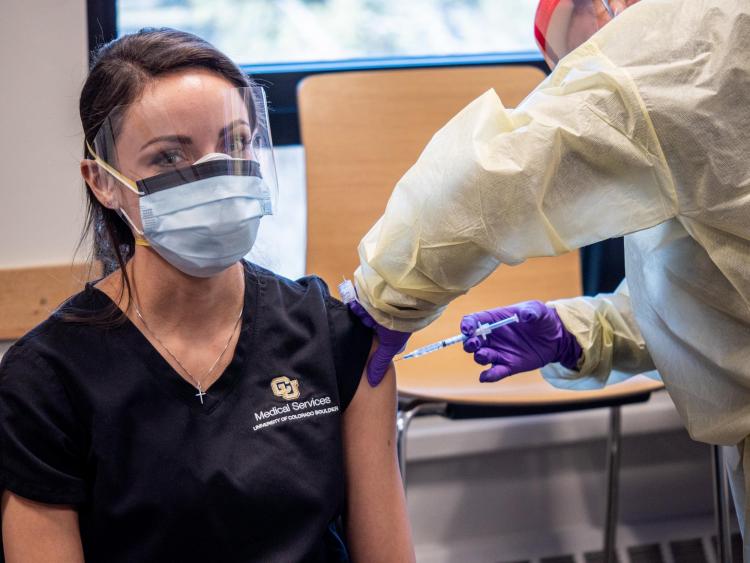
Registered nurse Katherine Noel prepares a dose of Moderna COVID-19 vaccine to give to staff at the Wardenburg Health Center on the CU Boulder campus. (Credit: Glenn Asakawa/CU Boulder)
With Moderna and Pfizer ramping up production, Johnson & Johnson poised to earn emergency use authorization from the Food and Drug Administration, and the White House promising 13.5 million vaccine doses per week to states, many see a light at the end of the COVID-19 tunnel.
As of Wednesday, 14.5% of Coloradans had gotten at least one shot and 6.8% were fully vaccinated.
“Through the use of vaccines, we have the ability to end this pandemic,” said Matt McQueen, director of epidemiology for the Pandemic Response Office at CU Boulder.
But with increased vaccine availability have also come questions about how they work and what they do and don’t do. CU Boulder Today caught up with McQueen, a professor of integrative physiology, to get some answers.
The Pfizer and Moderna vaccines are mRNA vaccines. What does that mean and how are they different than traditional vaccines?
mRNA (short for "messenger ribonucleic acid") vaccines are just a different way to deliver the instructions to our immune system to recognize this virus and mount a response. Traditional vaccines use a virus that has been attenuated, or weakened, so they don’t cause infection but trigger your body to develop antibodies toward it. Other vaccines, like the Johnson & Johnson vaccine, deliver a part of the SARS-CoV2 virus on an existing and harmless virus, called a vector.
mRNA vaccines, instead of sending the virus or bits of virus, just send the blueprint for part of the virus—the spike protein. The blueprint gets inside your cells, which then manufacture the spike protein, and when the body detects it, your body generates an immune response. The mRNA has a short lifetime inside your cells and does not, as rumored, make any change to your DNA. Instead, your cells make the spike protein just long enough for your immune system to learn what the virus will look like if you are ever exposed and be ready to fight it off.
Are these new mRNA vaccines safe?
Yes. Both the Pfizer and Moderna vaccines were approved for emergency use by the Federal Drug Administration (FDA). As part of the approval process, independent experts reviewed the data from approximately 33,000 individuals who received either vaccine and concluded that side effects were relatively mild and short-lived and the known and potential benefits of avoiding serious disease from coronavirus outweighed the risk. Since these vaccines have been approved, roughly 63 million doses have been administered and the vaccines continue to be monitored for safety.
Will I have side effects after getting the shots?
Some people do. Others don’t. Anecdotally, there seems to be a higher incidence of side effects of the second dose among younger people. That’s to be expected because a younger, more robust immune system will ramp up more of a response than an older immune system. Common symptoms include pain at the injection site, general fatigue and tiredness, headache and fever. It’s a normal reaction—just your immune system doing its job.

Matt McQueen
How effective are these vaccines?
There is a difference between preventing infection and protecting individuals from the consequences of infection. We know that all of these vaccines are remarkably effective in protecting individuals from the consequences of infection. In clinical trials, over 99% of people who have been fully vaccinated have not experienced any type of severe disease, including hospitalization or death.
But can I still get infected with COVID-19 after being vaccinated?
It’s possible, but unlikely. Early evidence suggests that in the rare case that someone is infected after being fully vaccinated, they experience a milder course of illness than they would have otherwise. For instance, if you were to have a mild disease without the vaccine, you may be completely asymptomatic once vaccinated. If you would have been hospitalized, or even died, you may have a mild or moderate course of disease instead. The vaccine essentially defangs the virus.
Does the vaccine prevent transmission of COVID-19?
Although the vaccine can’t prevent you from being exposed to an infected person, once the virus gets inside a vaccinated person’s body it is much less likely to replicate, or be copied and expanded, to levels that are dangerous to others. There are early reports out of the Israel Health Ministry that the vaccines are effective at preventing all infections—asymptomatic or otherwise, which is further evidence that these vaccines are effective at breaking chains of transmission.
Which vaccine should I get?
Every vaccine that has been approved by an international governing body is remarkably protective against severe disease, hospitalization and death. The safest thing you can do is to take the vaccine that becomes available to you when it becomes available to you.
How many people have already had COVID?
Models show that around 28% to 34% of Coloradans have been infected with COVID. That’s consistent with the country as a whole. In some areas, like the Dakotas, it may be closer to 50%. You layer vaccinations on top of that natural immunity and that is really going to help us move out of the acute phase of the pandemic.
How long will protection against COVID last?
From what we have seen so far, we know that the vaccine efficacy lasts at least eight to 10 months. But immune cell—called T-lymphocytes as well as B-lymphocytes—can stick around in the body for years, breaking into action quickly if the body ever encounters the same virus again. So, it’s likely that protection from severe disease and hospitalization could last for many years.
Does the vaccine protect against new COVID variants?
It is important to note that these mutations we are seeing do not turn the virus into some sort of super-survivable virus that has fundamentally new characteristics. Instead, the mutations to date appear to alter parts of the spike protein to enable it to bind more easily to the host receptor (ACE-2) of our cells. This could mean it is more infectious or spreads more easily. But there is growing evidence that existing vaccines are remarkably effective against these variants and provide protection against severe illness, hospitalization and death.
Brittany Delgado, a registered medical assistant at Wardenburg Health Center on the CU Boulder campus, was one of several medical staff that received the first of two Moderna COVID-19 vaccinations on Tuesday, January 5, 2021. (Credit: Glenn Asakawa/CU Boulder)
Once you are fully vaccinated, what can and can’t you do?
Once vaccinated, CU Boulder faculty, staff and students should continue to follow campus health and safety guidelines as they pertain to masks, physical distancing, etc.
However, within groups of those who have been vaccinated (14 days after the second dose), it is entirely reasonable to relax some of those pre-vaccine precautions. For example, a small indoor gathering without masks would be a low-risk activity when amongst a group of fully vaccinated individuals. Visiting family members who are also vaccinated would be another reasonable activity—and one that we are all longing for.
When will students, staff and faculty at CU Boulder be able to get vaccinated?
We have been able to vaccinate a number of our frontline health care workers and will continue to expand access as supply chain and prioritization allows. We are hopeful we can begin widespread vaccinations before the end of spring semester 2021.
What do you forecast for the next few months as far as the pandemic goes?
When you start getting past May and into June, we are going to enter a very new phase of this pandemic. Our hospitals will be emptied of COVID patients as we continue to vaccinate our most vulnerable. COVID deaths will be plummeting because over 60% of the population, largely adults who are at higher risk, will have protection from disease. My prediction is that the summer of 2021 will look a lot more like the summer of 2019 than the summer of 2020.
How will this pandemic end?
We have about 200 circulating respiratory viruses in the world, and it’s possible that SARS COV-2 will just become one of the many. However, through natural and vaccine-induced immunity, infections are likely to be mild and indistinguishable from other “common cold” coronavirus infections.


